To read the buzz in the press these days, one might think so.
A few months ago, I posted a story about vitamin D and breast cancer. It was a post discussing a report presented at this year’s meeting of the American Society of Clinical Oncology that showed that although vitamin D may not prevent the development of breast cancer, there seems to be a correlation between vitamin D levels and distant disease-free survival (the percentage of women alive with no evidence of spread of their disease) in women who develop the disease.
This prompted some interesting discussion in the comments, with one reader talking about taking vitamin D supplements and another expressing concern that people would start taking supplements without understanding potential consequences. Yet another reader, Ryan W., raised the question about whether vitamin D levels alone exert the observed effects, or whether what is really being seen is an interaction between vitamin D and infection/inflammation as discussed in this blog post. These are great points and questions – so I thought I would address some of them.
First of all, vitamin D metabolism is very complicated.
This graphic, borrowed from an excellent website by the University of Washington, shows how vitamin D is made from cholesterol in the liver and activated by sunlight in the skin and then further activated by the liver and kidneys to make the active form, 1, 25 (OH)2 vitamin D. This active form binds to a protein found inside vitamin D-responsive cells called the Vitamin D Receptor. The complex between 1, 25 (OH)2-vitamin D and its receptor then enters the nucleus and changes the activity level of dozens (if not hundreds) of genes. Most of the so-called vitamin D target genes have not yet been identified, so the specific mechanism by which vitamin D does anything, from regulating calcium metabolism to influencing the immune system is not known.
Regardless of how it happens, more and more research is demonstrating beneficial effects of vitamin D in patients with colorectal carcinoma. Just last year, a study was published showing a correlation between vitamin D levels and the risk of developing colorectal carcinoma. This was a type of study called a meta-analysis, which combines the results of several smaller studies to strengthen the statistical support for the conclusion. In this particular report, the results of 5 previously published studies on the correlation between vitamin D and the development of colorectal carcinoma were analyzed together.
Figure 2 of that report, reproduced here, shows that when data from all 5 previous reports are combined, they show a significant (almost 50%) drop in the rate of colorectal carcinoma in the patients with the highest blood vitamin D levels compared to the patients with the lowest levels.
This does not mean that taking vitamin D supplements can necessarily decrease your risk of getting cancer. It only shows that people who have higher vitamin D levels are less likely to get this particular type of cancer. It shows a correlation, but the cause could be from something else entirely. However, another study published last year suggests that the effect may really derive from vitamin D itself. In this study, 1180 white women older than 55 and in otherwise good health were randomly assigned to one of three groups: 1) placebo, 2) calcium supplementation with a vitamin D placebo, or 3) supplementation with both calcium and vitamin D.
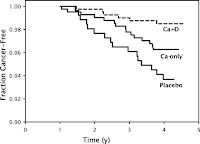 Figure 2 from their paper shows the fraction of women without cancer among the three groups. The group that took both vitamin D and calcium supplementation developed cancer at a lower rate than either of the other two groups.
Figure 2 from their paper shows the fraction of women without cancer among the three groups. The group that took both vitamin D and calcium supplementation developed cancer at a lower rate than either of the other two groups.
Just last month, another paper in the Journal of Clinical Oncology was published showing a beneficial relationship between vitamin D and survival from colorectal cancer. In this case, the investigators examined the correlation between prediagnosis vitamin D levels and survival among 304 participants in the Nurses’ Health Study and the Health Professionals Follow-Up Study who were diagnosed with colorectal cancer from 1991 to 2002. They found that higher vitamin D levels in the blood were correlated with improved overall survival.
So does this mean that we should all start taking vitamin D supplements? I don’t think so. First of all, it remains unclear how vitamin D impacts on the development of cancer and on the survival of cancer patients. Other than the study of white women from Nebraska, none of the reports is an “intervention study.” This means that one factor (vitamin D level) was compared with another (survival). A study like this can’t possibly prove that the one causes the other. Maybe the people with high vitamin D levels have better overall eating habits or exercise more in the sun, or have genetic difference in the way that their body metabolizes vitamin D. Any of these might also influence survival and would NOT be duplicated by taking a supplement.
How about the supplement study? The major limitation there is that subjects were all post-menopausal white women from Nebraska. Whether supplementation will help any other population is not clear at all.
Also, as with all other facets of nutrition, too much of a good thing can be a bad thing.
Too much vitamin D can hurt peripheral arteries, causing calcium deposition and inflammation and decreasing their elasticity. Excess vitamin D, if it results in excess serum calcium, can also contribute to the development of kidney stones. So, please, before taking any supplement, please check with your health care provider to determine if this is right for you and your specific medical history.
Regardless of whether or not supplementation is warranted, recent studies do all point to the same thing: vitamin D probably has effects on your body far beyond bone health. Future work will hopefully clarify how vitamin D affects the development of cancer and survival once cancer is diagnosed.
Related Posts:
Does Vitamin D Prevent Breast Cancer?
What’s New in Cancer Research?
Breast Cancer Risk & Alcohol









8 comments:
Readers may find the animated diagrams here http://www.uvguide.co.uk/vitdpathway.htm an easier representation of Vitamin D photosynthesis.
When considering vitamin D status the starting point should be IMO "What is the NATURAL Level our bodies evolved to attain and maintain?"
Is the level at which vitamin d flows in breast milk a sensible indicator?
Who thinks breast milk should not naturally contain vitamin d3? Please provide reasons for your choice.
Heaney has show the human body uses up to 5000iu/daily. http://www.ajcn.org/cgi/content/full/77/1/204 That represents a 25(OH)D of 50ng 125nmol/l Does ensuring your bodies daily needs are met sound a reasonable position to start from?
Hollis has shown that once the bodies daily needs are met the body's store of Vitamin D3 increases. Is this further evidence that 50ng 125nmol/l should be considered as the base level we should strive to attain and maintain?
Garland has shown that the lowest incidence of breast/colon cancer seems to occur around 52ng 130nmol/l. Is this further evidence that once the bodies daily needs have been met and some stores of vit d acquired the body is better able to deal with the challenge of cancer?
There is good scientific evidence dating from prewar studies showing peak muscle performance occurs only around 50ng 125nmol/l. Is this a sensible indicator of Vitamin D sufficiency?
The UK average 25(OH)D status is 50nmol/l 20ng that represent a total intake of 2000iu/daily over the year from sunlight/diet/supplements.
To achieve the lowest sensible threshold of Vitamin D sufficiency 80nmol/l (the level at which most but not all people absorb optimal amounts of calcium from the diet) would require an additional 1200iu/daily supplementation. Each 1000iu/daily/d3 raises 10ng 25nmol/l
To achieve optimal status IMO the level at which nature evolution shows provides sufficient reserves to both meet our daily needs fully and leave a surplus to deal with cancer or other challenge to the immune system is 130nmol/l 52ng and this requires the average UK adult to take a supplement/or acquire from sunlight an additional 3000iu/daily.
Lab, animal, and some preliminary human studies suggest that vitamin D may be able to protect against some cancers. Several studies suggest that a higher dietary intake of calcium and vitamin D correlates with lower incidence of cancer.44-51 In fact, for over 60 years researchers have observed that greater sun exposure reduces cancer deaths. Benefits of Vitamin D
Ted - Does ensuring your bodies daily needs are met sound a reasonable position to start from?
The problem with this reasoning is that calciferol and related chemicals are better viewed as hormones rather than vitamins.
High levels have long term risks, including calcification, as the OP mentioned. Also, since infection upregulates the production of 1,25D from 25D it's worth asking whether low 25D is just a symptom of infection rather than a 'deficiency' in its own right. Low 25D and high 1,25D would indicate infection rather than deficiency.
Any new studies going on now?
Hey Doc,
This was all so interesting. Now I have a question. I've recently been told I was deficient in Vitamin D? I'm out in the sun, and I drink milk daily.
Any explanation? I was told to take 800 units(?) a day for 3 months now.
Sounds right?
Thanks!! (mom of son with BT)
Susan, like you I was told I was deficient, I was put on a prescription form.
.. a bit more than 800 units though .... rolls eyes ...
whoops ..rolling eyes at myself, not at susan ... embarrassed at having to take so much ...
Hi thannks for posting this
Post a Comment